History of Present Illness: 18 year old female presents with a worsening neck mass over the last few weeks.
- Three weeks weeks ago, she reports initially having fevers, aches, chills and severe sore throat.
- One week ago, she was seen in the clinic for sore throat and neck swelling and had a Monospot test which was negative
- Diagnosed with probable viral syndrome and was placed on a Medrol dose pack for the neck swelling.
- After some initial improvement, the pain, swelling and redness worsened, prompting her visit to the ED
- Review of systems: She denies any fever, chills. Other than above history, she did report a rash for 2-3days about 3 weeks ago. She didn’t notice any shortness of breath or cough until day of ED visit. She did recent dental work, no TB exposure
Past Medical History:
- Seizure disorder – partial seizures, seizure free for last 2 years
- Urinary tract infection 2 months ago with admission for IV/Abx
- No Previous History of Mononucleosis
Meds:
- Lamictal 100mg BID
- Prednisone taper
Social: No ETOH, No Smoking, College Freshman
Physical Examination:
- Vital Signs: Temperature 97.7, pulse 54, Respiratory 18, Pox 88%, 105/68
- Gen: A/O, nontoxic appearing
- HEENT: No thrush, No dental
- Neck: Significant fullness Left Neck with mild erythema, some fluctuance. Mild lymphadenopathy below mass in L. ant cervical chain.
- Chest: L clear, HS1S2
- Abdomen: No splenomegaly
- Ext: Benign.
Laboratory Evaluation:
- WBC: 18.44 Segs 75, Lymphs 19
- H/H: 10.6/31.9 Platelet 360
- BMP normal
Radiology:

Questions:
- What was/were the most likely risk factor(s) for the evolution of this process
- The use of the steroid taper
- Underlying viral syndrome per history
- Her Lamictal led to an immunocompromised state
- What studies are missing in the work-up (hint: look at vital signs)?
- Why may she not have had a fever?
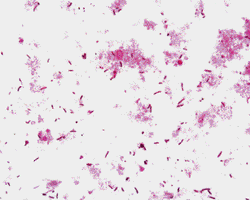
- What is the likely diagnosis (Gram stain below) and the organism associated with it?

Feel free to leave a comment of any or all of the answers.
Answer is provided in the link below:
https://yourhealthforumbydrcirino.org/2019/08/31/18-year-old-with-increasing-neck-mass/




Leave a Reply